Equine Metabolic Syndrome (EMS): A Common Cause of Laminitis in Horses and Ponies
Dr Brianna Clark
Equine Internal Medicine Specialist
Sunshine Coast Equine Hospital
Every year we see the same concerning scenario.
A flush of green grass appears… and a previously sound horse becomes foot sore.
Or a well-managed performance horse starts turning short, feels uncomfortable after trimming, or just seems subtly “off”.
These are often early signs of laminitis, and one of the most common underlying causes is Equine Metabolic Syndrome (EMS).
EMS is increasingly recognised across many breeds, and while it is manageable, management is often not simple. Successful treatment almost always requires an individualised, long-term management plan.
What is Laminitis?
Divergent hoof rings showing previous laminitis
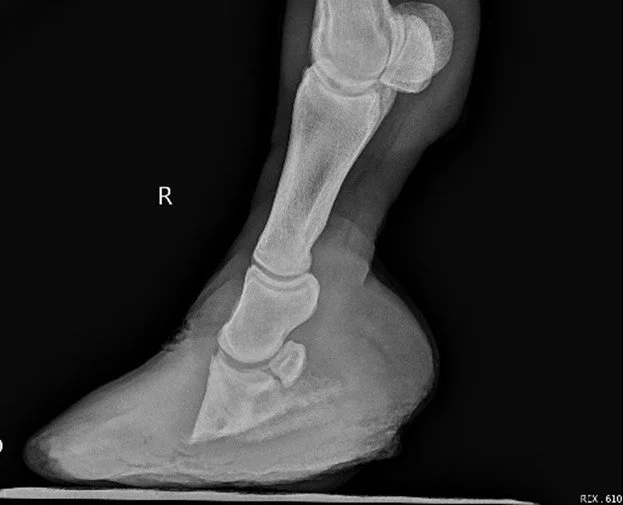
Laminitis is a painful condition affecting the structures that suspend the pedal bone inside the hoof.
When these attachments weaken, the pedal bone can rotate or sink within the hoof capsule, causing significant pain and long-term structural damage.
Laminitis ranges from:
Mild, intermittent soreness
Recurrent low-grade episodes
Severe, acute lameness
Even subtle cases matter. Repeated low-grade laminitis can permanently alter hoof structure and performance ability.
What is Equine Metabolic Syndrome?
Equine Metabolic Syndrome is an endocrine disorder and is the most common cause of laminitis.
The defining feature of EMS is insulin dysregulation, which includes:
Abnormally high circulating insulin levels (hyperinsulinaemia)
Insulin resistance, where body tissues respond poorly to insulin
Importantly, elevated insulin alone can trigger laminitis, even without grain overload or illness.
EMS commonly occurs alongside increased body fat deposition, but not all affected horses appear obviously overweight.
It’s not just ponies
Ponies remain highly represented, but EMS is not limited to pony breeds.
We now regularly diagnose EMS in:
Warmbloods
Andalusians
Arabians
Certain bloodlines appear more metabolically efficient and therefore more susceptible.
In modern management systems, with improved nutrition, reduced workload and abundant pasture, genetically efficient horses may struggle to regulate metabolism appropriately.
Why EMS can be difficult to manage
One of the most important things owners should understand is:
EMS management is rarely a quick fix.
While the principles are well established, every horse responds differently.
Challenges commonly include:
Variable insulin responses between individuals
Differences in pasture tolerance
Weight loss resistance
Concurrent conditions such as PPID
Owner lifestyle and property limitations
For this reason, successful management almost always requires a tailored, individualised treatment plan developed with your veterinarian and adjusted over time.
Subtle signs owners often miss
Endocrine laminitis is frequently insidious rather than dramatic.
Common early signs include:
Foot soreness after farriery
Shortened stride or reluctance to turn
Increased digital pulses
Recurrent hoof abscesses
Changes in hoof growth rings
Fat pads over the crest, shoulders or tail head
A firm or enlarged crest
Early investigation can prevent significant hoof damage.
Assessing body condition - more than just weight
Welsh B with a BCS of 6/9 and CNS of 3/5
We evaluate metabolic risk using two scoring systems:
Body Condition Score (BCS)
Scale 1–9
Ideal: 5–6/9
Cresty Neck Score (CNS)
Scale 0–5
Ideal: ≤2/5
Regional fat deposits, particularly along the crest, are metabolically active and strongly linked with insulin dysregulation.
Importantly:
Fat is not muscle, regardless of discipline or show conditioning standards.
How do we test for EMS?
Diagnosis involves more than a single resting blood test.
At Sunshine Coast Equine Hospital, endocrine assessment typically includes:
Comprehensive clinical examination
Laminitis evaluation (often including radiographs)
Weight measurement and body condition assessment
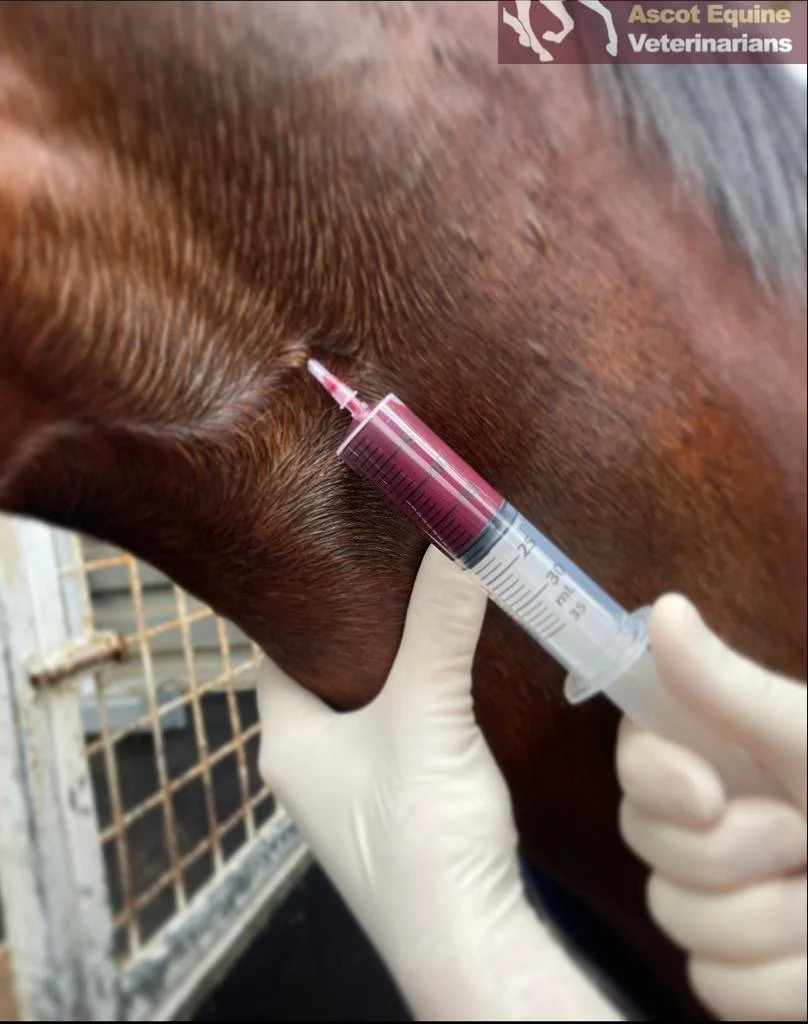
Dynamic metabolic testing
Because insulin abnormalities occur after eating, dynamic tests provide the most accurate information. These may include:
Oral Sugar Test (OST)
Oral Glucose Test (OGT)
These tests safely assess how your horse’s insulin responds to dietary sugar, the key driver of endocrinopathic laminitis.
What about Cushing’s disease (PPID)?
Pituitary Pars Intermedia Dysfunction (PPID), commonly called Equine Cushing’s disease, is a separate endocrine condition that frequently overlaps with EMS.
Testing is recommended in horses over approximately 12 years old, especially if you notice:
Delayed coat shedding
Muscle loss
Lethargy
Recurrent infections
Laminitis episodes
Patchy or reduced sweating
Managing both conditions together is often essential for success.
Managing EMS: a long-term approach
EMS management focuses on reducing laminitis risk and improving insulin regulation.
There is no universal protocol, management must be adapted to each horse.
1. Nutrition: The Foundation
Dietary control remains the most important treatment.
Typical recommendations include:
Roughage intake around 1.5% of bodyweight daily
Hay containing <10% non-structural carbohydrates (NSC)
Practical strategies:
Weigh hay using luggage scales
Test forage where possible or purchase hay that has been tested to have low NSC content
Soak hay to reduce sugar content if required
Restrict or eliminate pasture access when necessary
Avoid treats, feed scraps and hidden sugars
Even short periods on lush pasture can deliver large carbohydrate loads.
2. Exercise
Exercise improves insulin sensitivity and supports weight management.
However:
Horses should not be exercised during active laminitis.
Once comfortable, carefully introduced exercise becomes an important part of long-term management.
3. Farriery collaboration
Successful cases rely on strong communication between veterinarian and farrier.
Radiograph-guided trimming can greatly improve comfort, hoof mechanics and long-term outcomes.
4. Medication - when needed
Medication may be introduced when dietary management alone does not sufficiently control insulin levels.
Common options include:
Ertugliflozin – decreases insulin levels released from the pancreas
Metformin - reduces intestinal glucose absorption
Levothyroxine - supports weight loss and metabolic rate
Medication is an adjunct to management, not a replacement for dietary control.
Prevention and early screening
Many horses live with insulin dysregulation for years before developing obvious laminitis.
Early endocrine testing allows:
Identification of at-risk horses
Preventative management
Reduced likelihood of future laminitis episodes
Proactive assessment is particularly valuable for predisposed breeds and individuals with regional adiposity.
The take-home message
Equine Metabolic Syndrome is common across both horses and ponies.
It can be challenging to manage, but with careful monitoring, tailored treatment and veterinary guidance, affected horses can live comfortable and athletic lives.
Early recognition is key.
Book an Endocrine Assessment
If your horse or pony has experienced laminitis, struggles with weight control, or shows signs of metabolic disease, a structured endocrine evaluation can help guide management.
Sunshine Coast Equine Hospital offers comprehensive endocrine assessments tailored to the individual horse.
Book an Endocrine Assessment with our team today
Contact Sunshine Coast Equine Hospital to arrange an appointment or discuss whether testing is appropriate for your horse.